Childhood Shots Aren’t Forever: Why Adult Boosters Matter
Most adults assume the inoculations they received in school will shield them for a lifetime, yet scientific evidence shows that immunity can diminish over the years. This article explains why revisiting vaccination status in adulthood, especially for diseases such as pneumonia, shingles, and hepatitis, is crucial for staying protected.
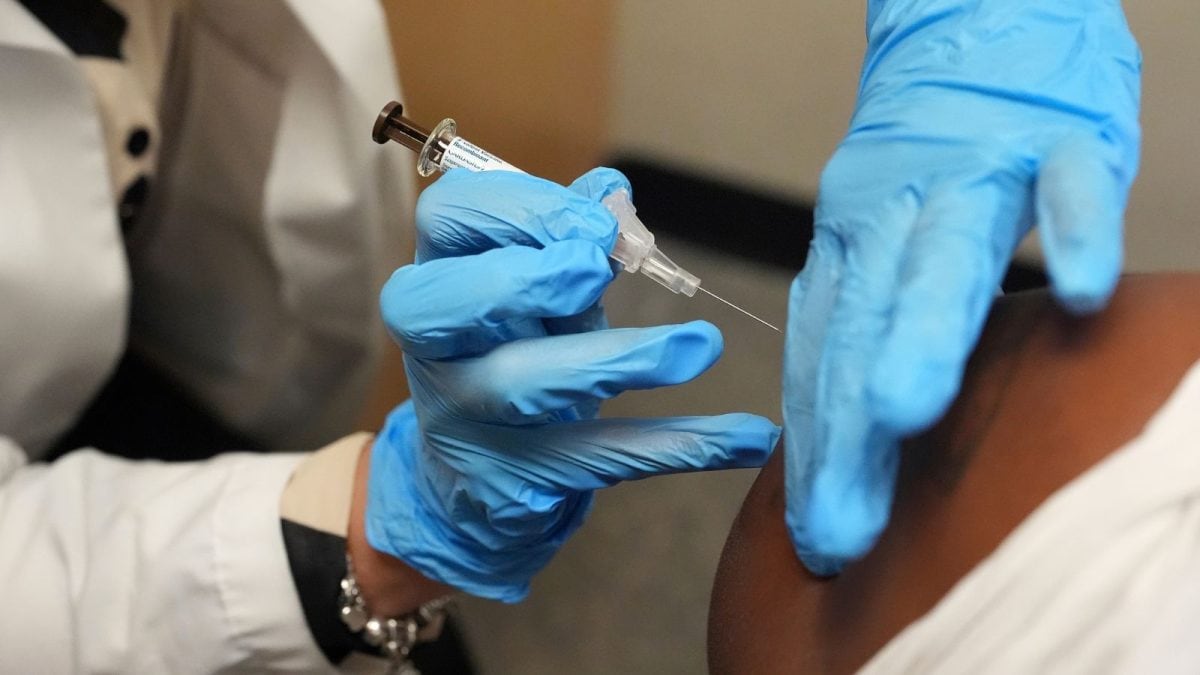
Most adults assume childhood vaccines last for life but immunity can fade. Why adult vaccination, boosters, against diseases like pneumonia, shingles and hepatitis matter now
Remembering the Needle in School
Think back to the moment you sat in a school infirmary, felt the quick sting of a needle, and left with a sore arm that faded after a day. After that brief encounter, no follow‑up calls arrived, no reminder cards were mailed, and life continued unchanged. The impression that the job was finished stayed with many adults for decades.
For a handful of illnesses, a single dose during childhood truly provides lifelong protection. For the majority, however, the vaccine‑induced shield is not a static barrier; it is a dynamic response that can wane as time passes.
Dr (Col) Vijay Dutta, Director, Internal Medicine & Respiratory Services, ISIC Healthcare explains that many adults underestimate the fact that several childhood immunizations were never designed to protect indefinitely. The immunity granted by those shots is genuine, yet, just like any other physiological process, it may gradually diminish without periodic reinforcement.
Recognizing this natural decline does not demand panic. Instead, it invites a straightforward question that most people never consider asking their primary care provider: "Am I still adequately protected against these diseases?"
Why the Issue Grows More Pressing With Age
Children receive vaccines while their immune systems are still learning to recognize and neutralize pathogens. Immunological memory is not a set‑and‑forget mechanism; it constantly evolves throughout a person’s life. As the body ages, the immune response remodels, often becoming less vigorous. Infections that caused only minor inconvenience in early adulthood can turn serious, or even life‑threatening, when encountered in later decades.
Dr (Col) Vijay Dutta points out that illnesses such as pneumonia, shingles, whooping cough, and hepatitis are not exclusive to the elderly or chronically ill. They also affect adults who mistakenly believe they remain protected because they were vaccinated decades ago.
Adding to the complexity, the microbial landscape itself has shifted. New viral strains emerge, and older pathogens reappear in altered forms. The contemporary disease environment therefore differs markedly from the one that shaped the childhood vaccine schedule for earlier generations.
The Hidden Gaps in Adult Immunity
Dr (Col) Vijay Dutta highlights several categories of gaps that many people are unaware of:
- Waning protection: Some vaccines lose potency over time, making booster doses essential to sustain effectiveness.
- Absent childhood doses: A variety of vaccines now recommended for adults were not part of the routine schedule when older generations were children.
- Age‑specific relevance: Certain vaccines become particularly important after reaching specific age thresholds, often around the fifth decade of life, or when a chronic condition alters vulnerability.
- Lifestyle‑driven needs: Factors such as international travel, pregnancy, or managing long‑term conditions like diabetes can create additional immunization gaps.
These gaps are more common than most people realize, and they exist across a broad spectrum of diseases, from respiratory infections to hepatitis and beyond.
Practical Steps to Close the Gaps
According to Dr (Col) Vijay Dutta, addressing these gaps does not require a marathon of medical appointments. In many cases, a single conversation with a healthcare professional can identify the necessary catch‑up vaccines, followed by one or two visits to receive them.
"The vaccines that frequently emerge for adults who have not reviewed their immunization status in years include protection against pneumococcal disease, shingles, tetanus, hepatitis B, and seasonal influenza," says Dr (Col) Vijay Dutta. "Most individuals are genuinely surprised to discover that these vaccines are both safe and specifically relevant to them, simply because the topic never arose during routine care."
Timing also plays a strategic role. Some vaccines achieve optimal benefit when administered before the onset of infection seasons, while others are most advantageous at distinct life stages. Initiating the conversation early expands the range of options and ensures that vaccines are given at the most effective moments.
Adopting an Ongoing, Proactive Immunization Mindset
Dr (Col) Vijay Dutta outlines a concise checklist for adults seeking to maintain robust protection:
- Do not assume that childhood vaccines provide lifelong coverage for every disease.
- Ask a healthcare professional about adult immunization needs even when not currently ill.
- If over fifty years of age, or if managing a chronic health condition, prioritize a review of vaccine status.
- Encourage older family members, especially aging parents, to assess their immunization gaps as well.
- Recognize that feeling healthy does not automatically equate to being immunologically protected.
Dr (Col) Vijay Dutta emphasizes that immunity is a continuous conversation, not a chapter closed in childhood. For many of the infections that acquire greater significance in adult life, revisiting vaccination is a practical, low‑burden strategy that can dramatically improve health outcomes.
The shot administered at ten years old may have performed admirably at the time. The essential question today is whether that same dose continues to offer the intended shield, or whether a booster—or an entirely new vaccine—has become necessary.







